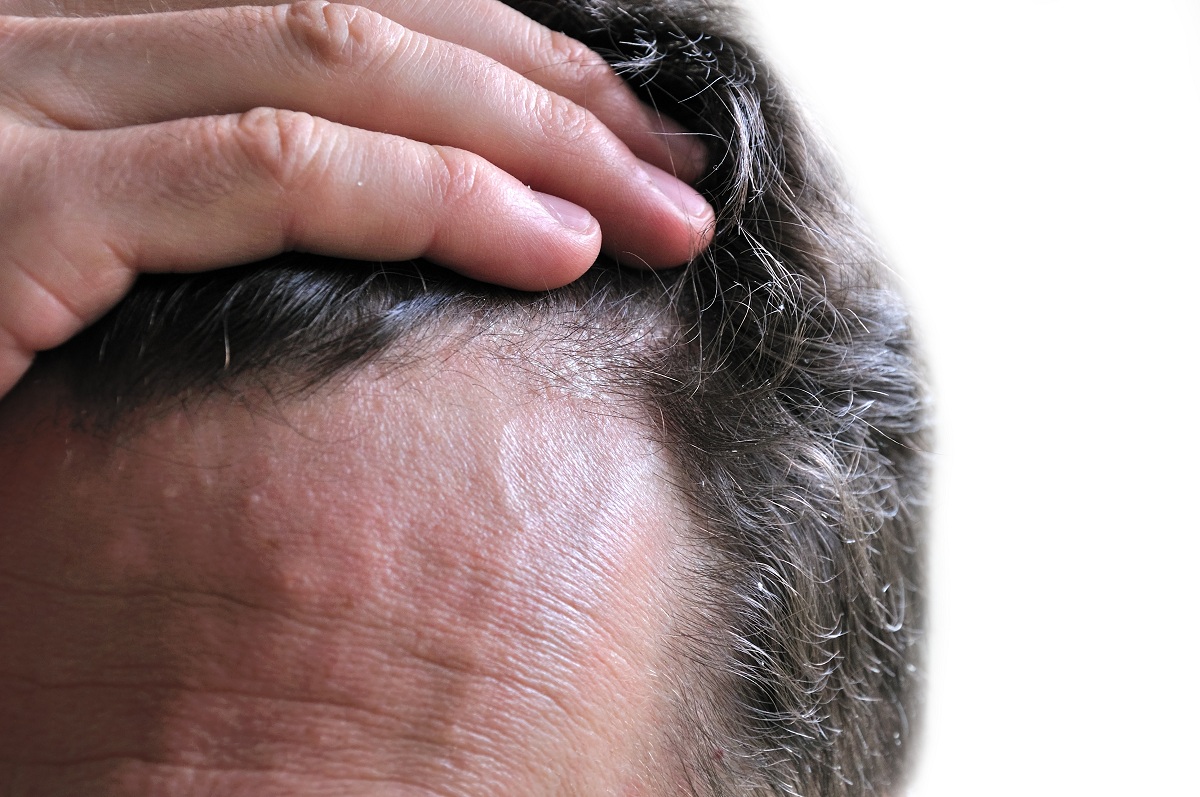
Seborrheic dermatitis is a papulosquamous disorder patterned on the sebum-rich areas of the scalp, face, and trunk (see the image below). In addition to sebum, this dermatitis is linked to Malassezia, immunologic abnormalities, and activation of complement. Its severity ranges from mild dandruff to exfoliative erythroderma.
Contents
Signs and symptoms
History findings in seborrheic dermatitis may include the following:
- Intermittent, active phases manifesting with burning, scaling, and itching, alternating with inactive periods; activity is increased in winter and early spring, with remissions commonly occurring in summer. This may be from sunlight effect on Malassezia.
- In active phases, potential secondary infection in intertriginous areas and on the eyelids
- Candidal overgrowth (common in infantile “napkin dermatitis”)
- Generalized seborrheic erythroderma (rare)
Physical findings may include the following:
- Scalp appearance ranging from mild, patchy scaling to widespread, thick, adherent crusts; plaques are rare; lesions may spread from the scalp onto the forehead, the posterior part of the neck, and the postauricular skin
- Seborrheic skin lesions manifesting as scaling over red, inflamed skin; hypopigmentation (in blacks); oozing and crusting; blepharitis (occurring independently)
- Lesion distribution following the oily and hair-bearing areas of the head and the neck; extension to submental skin can occur
- Either of two distinct truncal patterns: annular or geographic petaloid scaling or pityriasiform variety (rare)
Malassezia organisms are probably not the cause of seborrheic dermatitis but a cofactor linked to a T-cell depression, increased sebum levels, and an activation of the alternative complement pathway. Various medications may also flare or induce seborrheic dermatitis.
Causes
We don’t know what exactly causes seborrheic dermatitis. It seems to be a combination of things, including:
- Stress
- Your genes
- A yeast that normally lives on skin
- Certain medical conditions and medicines
- Cold, dry weather
It doesn’t come from an allergy or being unclean.
Newborns and adults aged 30-60 are more likely to get seborrheic dermatitis. It’s more common in men than women and in people with oily skin. These medical conditions can also raise your risk:
- Acne
- AIDS
- Alcoholism
- Depression
- Eating disorders
- Epilepsy
- Heart attack or stroke recovery
- Parkinson’s disease
- Psoriasis
- Rosacea
Remedies
Fish oil
Fish oil supplements can help suppress flare-ups of dermatitis triggered by allergies. Fish oil has other nutritional qualities, as well. It’s recommended for overall immune and cardiovascular health because of its omega-3 fatty acids.
Aloe vera
Aloe vera is a plant with anti-inflammatory properties. Research has shown that its extract is effective in treating seborrheic dermatitis. Supplements containing aloe vera gel or extracts can help suppress flare-ups of SD. They can also lessen the severity of flare-ups that do happen.
Probiotics
Probiotics are sometimes recommended to treat different kinds of dermatitis, especially in children. But there is little research to link probiotics to effective results for SD. Still, probiotics can promote a healthier digestive system. This can decrease inflammatory issues throughout your body.
Honey
Honey is a potent broad spectrum antibacterial and anti-fungal food. It works a treat for removing the fungus that causes seborrheic dermatitis, both internally and topically.
A recent study proves this… In the study, 20 male patients and 10 females between the ages of 15 and 60 years with seborrheic dermatitis symptoms, including scaling, itching and hair loss, were instructed to apply diluted crude honey (90% honey diluted in warm water) every second day on their lesions by gently rubbing for a period of 2-3 minutes. After 3 hours, the honey was rinsed off with warm water. The patients were then monitored for changes in itching, scaling, hair loss and lesions during the treatment period of 4 weeks.
Treatment
Seborrheic dermatitis may go away without treatment. Or you may need many repeated treatments before the symptoms go away. And they may return later. Daily cleansing with a gentle soap and shampoo can help reduce oiliness and dead skin buildup.
Seborrheic dermatitis is also called dandruff, seborrheic eczema and seborrheic psoriasis. For infants, the condition is known as cradle cap and causes crusty, scaly patches on the scalp.
Medicated shampoos, creams and lotions are the main treatments for seborrheic dermatitis. Your doctor will likely recommend you try home remedies, such as over-the-counter dandruff shampoos, before considering prescription remedies. If home remedies don’t help, talk with your doctor about trying these treatments.
Creams, shampoos or ointments that control inflammation
Prescription-strength hydrocortisone, fluocinolone (Capex, Synalar), clobetasol (Clobex, Cormax) and desonide (Desowen, Desonate) are corticosteroids you apply to the scalp or other affected area. They are effective and easy to use, but should be used sparingly. If used for many weeks or months without a break, they can cause side effects, such as thinning skin or skin showing streaks or lines.
Antifungal gels, creams or shampoos alternated with another medication
Depending on the affected area and the severity of your symptoms, your doctor might prescribe a product with 2 percent ketoconazole (Nizoral) or 1 percent ciclopirox. Or you doctor may prescribe both products to be used alternately.
Antifungal medication you take as a pill
If your condition isn’t improving with other treatments, your doctor may recommend an antifungal medication in pill form. These aren’t a first choice for treatment because of possible side effects and drug interactions.
